The development of technologies such as the telescope and microscope were transformational events in human history. They extended human perception to the far and the small, to the big and the near. Thereby upending our understanding of the universe and our place within it. Similarly, radiological imaging has extended our power of perception, not to the outside but inwards, rendering our insides transparent. They are modern medicines version of “windows into the soul” that promise to uncover deep, hidden, and lurking demons. In doing so, they have transformed medicine. X-ray technology, its offshoot Computed Tomography (CT), and Magnetic Resonance Imaging (MRI) are ubiquitous tools of contemporary medicine. They yield unprecedented insight into anatomy, physiology, and pathology. Fundamental actions in medicine – screening, diagnosis, prognosis, surveillance, treatment response – are afforded by imaging studies.
Although mostly with a focus on screening and diagnosis, radiological imaging is also a staple tool for the emergency physician. As a category, imaging studies are the second most frequent source of patient data in the emergency department, behind biomarker testing. In contrast to the few-to-many (biomarker-diagnosis) mapping of biomarkers, often rendering lab biomarkers non-specific, imaging studies offer the advantage (and disadvantage) of panoptic-like visualization of regional anatomy (i.e. abdomen, lower extremity, chest) which includes the organ of interest. For example, an X-ray will not only be diagnostic but also prognostic for a patient who falls and has a deformity on the physical exam. Or evidence of bleeding in the brain is diagnostic and prognostic in a patient who is confused with an elevated blood pressure. Radiological imaging – when clear – has the unparalleled potential to not only minimize cognitive expenditure by minimizing the requirement of interpretation and inference, but also to narrow the affordance space to an optimal few.
Unfortunately, patients in the emergency department only occasionally present with such clarity. More often than not, encounters are laden with ambiguity and hidden risk. The next best set of actions are interpretation and inference dependent, open and wide. They require knowledge of patient specific attributes, individual patient risk tolerance philosophies, and thresholds for treatment. The increased visibility of imaging studies also carries with it a dark side. It raises the specter of incidentalomas – findings noted to be incidental to the presentation or those that represent normal variants.
For example, a patient presenting with chest pain has findings on a chest x-ray that that could be pneumonia or pulmonary edema. Should they be treated for both, either, or neither? Or as another example, a patient with vague abdominal pain, a non-specific physical exam, and normal labs has a CT scan of the abdomen which shows findings of an adrenal mass or a marginally dilated appendix. Is the marginally dilated appendix the source of her symptoms? Should she be referred to the general surgeon for the marginally dilated appendix? What does adrenal mass mean for this patient? Does it require surveillance? Or the known scourge to the ED physician – the elderly patient with the interoceptive sensation of “dizziness.” Exam findings in such patients are reliably unreliable. Essentially grasping for security, the ED physician reaches for CT imaging to rule-out a high-morbidity diagnosis such as a brain hemorrhage, but knows full well that the test is insensitive to an ischemic stroke or a transient ischemic attack (TIA). If the CT happens to be normal and even if symptoms normalize, is the patient safe for discharge when neither an ischemic stroke or TIA is ruled-out?
Mandated with the task to screen and de-risk and recognizing the singular diagnostic power of radiological imaging, the frequency of imaging studies ordered in the ED have consistently increased and projected to continually increase. In-line with biomarker ordering, imaging studies are routinely ordered at triage as part of order sets. As more imaging studies are ordered, the number of incidentalomas and marginal findings will proportionally increase. If you factor in the general false-positive bias in healthcare, the default assumption of homogeneous patient values (future essay), and the lack of real understanding of fundamental patient heterogeneity (future essay), it will logically follow that these more marginal and irrelevant radiological findings will be acted up on with increasingly invasive diagnostic and treatment modalities leading to a cascading of false positives and iatrogenesis.
Discover more from S-Fxn
Subscribe to get the latest posts sent to your email.
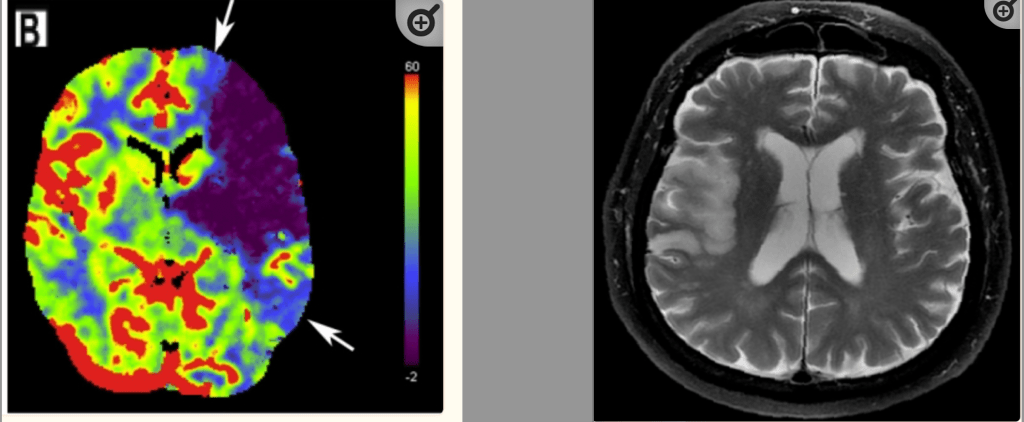
[…] pathological processes. Even if you only consider biology, the modern toolkit of biomarkers and radiological imaging afford only superficial legibility to the pathological processes that are occurring at the […]
[…] have made surgical interventions increasingly less traumatic and non-invasive. Advances in diagnostic imaging and biomarker testing have given us unparalleled access and insight into the anatomy, physiology, […]