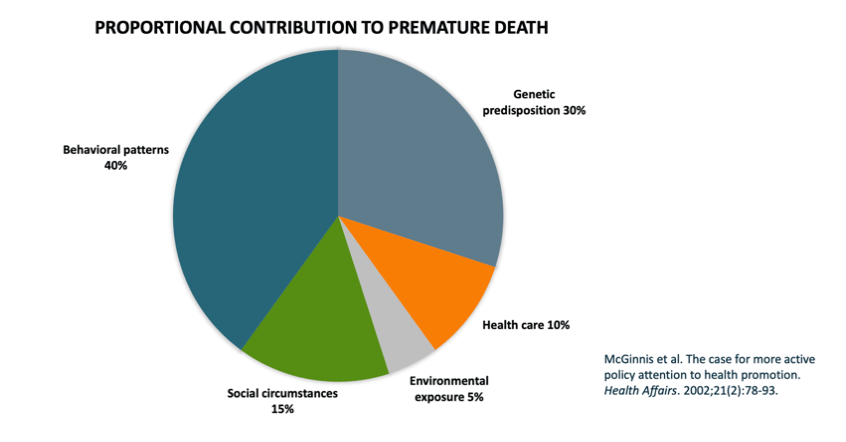
It has almost become a truism to attribute the causes of diseases to social determinants of health (SDOH). By one estimate, SDOH account for 60% of premature death in the United States. According to the CDC, SDOH are the conditions in the environments where people are born, live, learn, work, play, worship, and age. While the definition is inclusive of all of an individual’s environments , the CDC does group these social determinants into five more specific domains: economic stability, health care access and quality, education access and quality, neighborhood and built environment, and social and community context. These systems – operating on different but overlapping temporal, spatial, and power scales – have a disproportionate impact on health (and disease). In effect, these are the “networks above” that constrain and facilitate, incentivize and disincentivize, normalize and legitimize intentions and actions leading to differential and variable health outcomes between and within groups.
As these facts become internalized and incentive schemes such as value-based care are developed to reflect these facts, traditional storehouses of medical data such as health systems and insurance companies are beginning to create tools to unlock the predictive and prescriptive value of social data. The thesis being, marrying existing medical data that is stored in electronic health records to social data will yield insights that not only more precisely risk-stratify and sub-segment, but will also be more sensitive in detecting features that signal disease onset, trajectories, and outcomes. Therefore, intra-EHR screening tools are being created to collect individual level longitudinal data on homelessness, food insecurity, quality of nutrition, transportation barriers, educational gaps, lack of family and social supports, and neighborhood violence. However, self-reported data is limited by the fact that it only provides insight into intention and only partial insight into actions. Human psychology is such that intentions loosely and incompletely predict actions and individual perception of the environment is partially and often misaligned with reality. At best, these gaps lead to coarse grained or surface level predictions, and at worst, errant predictions.
In order to close these gaps, the parallel data streams should ideally be combined within the methodologies of network science and the dominant features of human networks – homophily and clustering. More specifically, medical data combined with individual level survey data, social media data, and community level data imported from public sources. For example, medical data such as medications, laboratory values, and problem lists should be merged with patient level screening tools that collect SDOH features such as activity levels, substance abuse, and feelings of safety, as well as community level data that includes statistics on neighborhood violence and the number of grocery stores, pharmacies, and public transportation options in the area. My thesis is that this synthesis of data sources will yield insights that are greater than the sum of the parts and narrow the gaps between intention, action, and outcome.
If the claim that SDOH significantly impact human health is true, then these data sources – the networks above – must be included in our models of human health and disease within the methodologies of network science. We must look beyond the person to the situation and beyond the intention to the action, to get a more complete map of human health. The person, their intentions (medical and social screening data), and the situation (community level data) are synergistic data sources when effectively combined, can yield better individual and population level insights. However, there is another lever that can be pulled to more fully bridge the gap between intention and action. Sensor technologies have multiplied across many realms of human activity from tracking devices in cars to online browsing. Data generated from these remote sources is another powerful data stream that has the potential to more fully bridge the gap between intention and action, especially when combined with medical data (next essay).
Discover more from S-Fxn
Subscribe to get the latest posts sent to your email.
[…] solution to minimize this limitation is to decompress and unpack medical documentation. Just like sensorization of the real world can complement patient intentions with actions by matching their interoceptive states with […]
[…] have remained intractable partly because the healthcare system nor medicine neither has the breadth or the depth of coverage to represent these pathological processes. Even if you only consider […]