How can we explain the observation that Pima Indians living in the Southwest United States have a five fold higher prevalence of diabetes than their counterparts living across the border in Mexico? Not only are these populations genetically identical, numerous studies have been unsuccessful in identifying chromosomal regions with a strong linkage to the trait. One’s genetics account for approximately 30% of the type 2 diabetes phenotype. It is speculated that the variation in disease prevalence is due to the environmental differences between the populations. Whereas, US Pima Indians have adopted a Western lifestyle of low physical activity and a “supermarket” diet, the Mexican Pima Indians remain as subsistence farmers with high levels of activity. However, what (if any) is the effect of the environment on the genome? What are the mechanisms that translate environmental exposures to the genome?
Humans respond to environmental challenges over a range of timescales. Firstly, there is a relatively static evolutionary component that proceeds over hundreds of generations and has minimal impact during an individual’s lifespan. Secondly, there are dynamic homeostatic alterations that occur over seconds or days in response to immediate challenges. Finally, there are epigenetic processes that adjust regulator mechanisms to changing environments that is the intermediate between that of evolution and homeostasis. The sum of the environment’s contribution to health (or disease) has been conceptualized as the exposome. These exposures are all encompassing and can be characterized as internal (ie metabolism, endogenous hormones, microbiome, inflammatory state), general external (ie education, financial status, stressors), or specific external (ie radiation, infectious agents, nutrition,  alcohol/tobacco). The overall relationship can be explained by the following equation: Phenotype = genotype X exposome. In the case of the Pima Indians, since we know the genotype is constant, it is exclusively the exposome that is causing the exaggerated disease burden for the US Pima Indians. In fact, the vast majority of our chronic disease burden can be explained by environmental factors that not only overwhelm our static genotype, but more importantly, our dynamic ability to maintain short and long term homeostasis. This dynamic nature of the exposome is also the most challenging feature of its characterization. Not only does a seemingly countless number of components need to be considered, but they also have to be understood in relation to their temporal variation. For example, at any given point in time, an individual will have a particular profile of exposures and this will change multiple times in a lifetime. Therefore, continuous data monitoring through extended periods of time is required to capture this information and find patterns of relationships. Sensors will play a key role in capturing this remotely generated physiological and environmental data. Isolated visits to the provider will not be sufficient to elucidate the complex relationships of the exposome. Mobile phones will serve as the hub for various captured data streams. For example, data captured from heterogeneous sources such as wearables/invisibles, social media streams, and environmental sensors will be integrated on the mobile phone. This information will then stream with clinical and genetic data on the electronic health record to create a data rich personal health record (PHR) that will provide highly individualized health (or disease) profile.
alcohol/tobacco). The overall relationship can be explained by the following equation: Phenotype = genotype X exposome. In the case of the Pima Indians, since we know the genotype is constant, it is exclusively the exposome that is causing the exaggerated disease burden for the US Pima Indians. In fact, the vast majority of our chronic disease burden can be explained by environmental factors that not only overwhelm our static genotype, but more importantly, our dynamic ability to maintain short and long term homeostasis. This dynamic nature of the exposome is also the most challenging feature of its characterization. Not only does a seemingly countless number of components need to be considered, but they also have to be understood in relation to their temporal variation. For example, at any given point in time, an individual will have a particular profile of exposures and this will change multiple times in a lifetime. Therefore, continuous data monitoring through extended periods of time is required to capture this information and find patterns of relationships. Sensors will play a key role in capturing this remotely generated physiological and environmental data. Isolated visits to the provider will not be sufficient to elucidate the complex relationships of the exposome. Mobile phones will serve as the hub for various captured data streams. For example, data captured from heterogeneous sources such as wearables/invisibles, social media streams, and environmental sensors will be integrated on the mobile phone. This information will then stream with clinical and genetic data on the electronic health record to create a data rich personal health record (PHR) that will provide highly individualized health (or disease) profile.
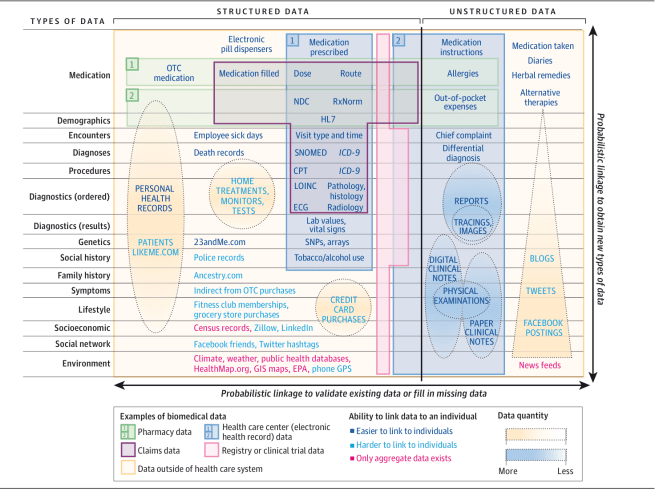
The scope and complexity of this undertaking is a massively formidable technological challenge (represented literally & figuratively in the infographic below) and is essentially a pipe dream at this time. To put this in perspective, this is not simply “big data analytics” but represents a time series of unstructured “big data” from heterogeneous sources. It will require novel biomarkers, continued exponential increase in processing power with concurrent miniaturization of sensors, and also will require an informatics infrastructure that will interface with these sensors. It will be able to curate and transform this data and present it as information in real time on PHR dashboards. Lastly (and maybe most importantly), we must not overlook the societal implications of intensive data sharing and remote monitoring. Our concepts of privacy and security will have to evolve to facilitate this new paradigm of information sharing. Forward thinking public policy will have to be developed to not only provide the necessary legal protections to consumers but also accommodate this shift to a data sharing and transparent society.
Sources:
- The Pima Indians: Pathfinders of Health
- Exposome Informatics: considerations for the design of future biomedical research information systems
- Finding the Missing Link for Big Biomedical Data
Discover more from S-Fxn
Subscribe to get the latest posts sent to your email.
[…] I talked about in an earlier post, human beings respond to environmental stimuli over a range of timescales. In between the slow […]
[…] The sum of the environment’s contribution to health (or disease) has been conceptualized as the exposome and until this can be further elucidated, these guidelines will be lacking granularity to […]
[…] system of interlocking feedback loops. We have only scratched the surface in modeling the exposome, and therefore, our predictions are predictably erroneous. The current gold standard of a sample […]